Benefits
Quality improvement
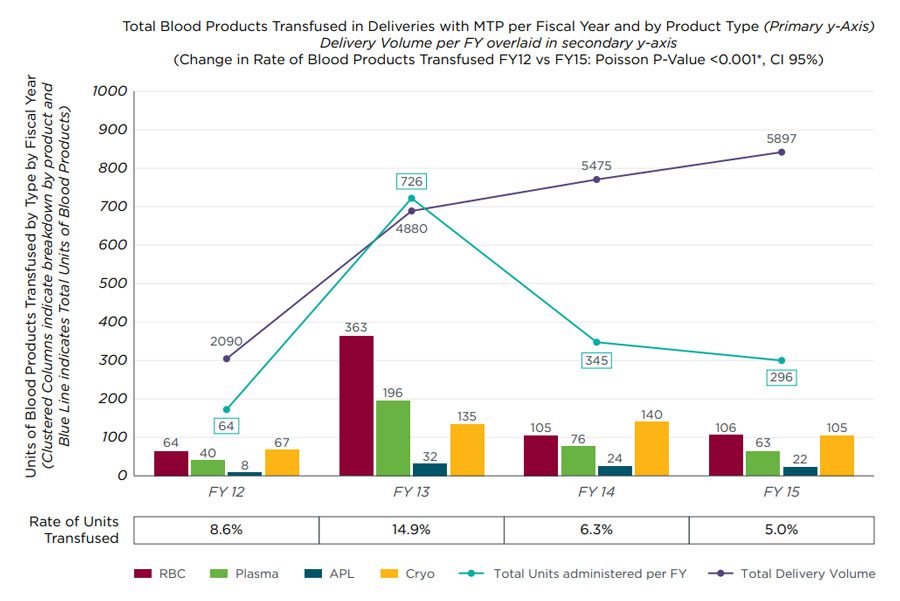
Increased patient safety was achieved through the standardization of clinical processes and reductions in care variation.
Maternal safety
64% decrease in obstetric adverse events (FY2012–FY2018).
Designation
Texas Children’s Hospital was one of the first three facilities in the state to earn designation as a level IV facility.