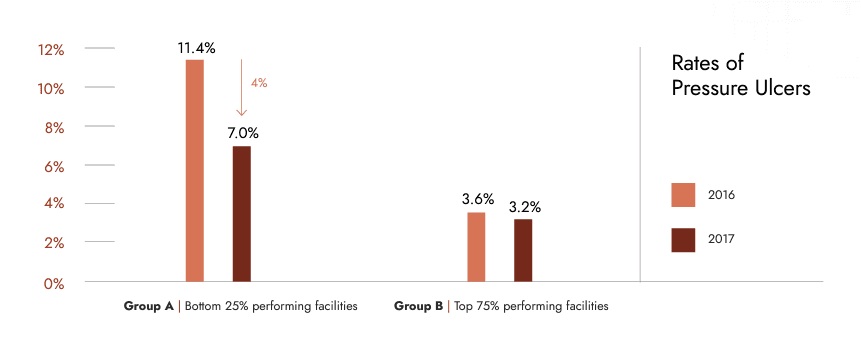
Improved outcomes
- Facilities, both with and without prior wound care training, experienced improvement in pressure injury rates of patients.
Cost savings
- Results indicated better wound care at an organization would save approximately $20,000 to $120,000 per injury.
Professional development
- 70% of 140 nurses passed the exam and became Wound Care certified.