Last month, we had the opportunity to partner with the National Council for Behavioral Health on the webinar, The Substance Use Professional of the 2020s.
Aaron Williams, Senior Director of Training and Technical Assistance for Substance Abuse, shared insights on:
- The current state of substance use in the U.S.
- The current landscape of substance use treatment
- The critical areas of knowledge development for substance use counselors
In short, the webinar gives those currently working in substance use and addiction treatment an idea of what is happening now and what to expect in the coming decade, including the core competencies needed for effective practice in 2020 and beyond.
The Current State of Substance Use in the U.S.
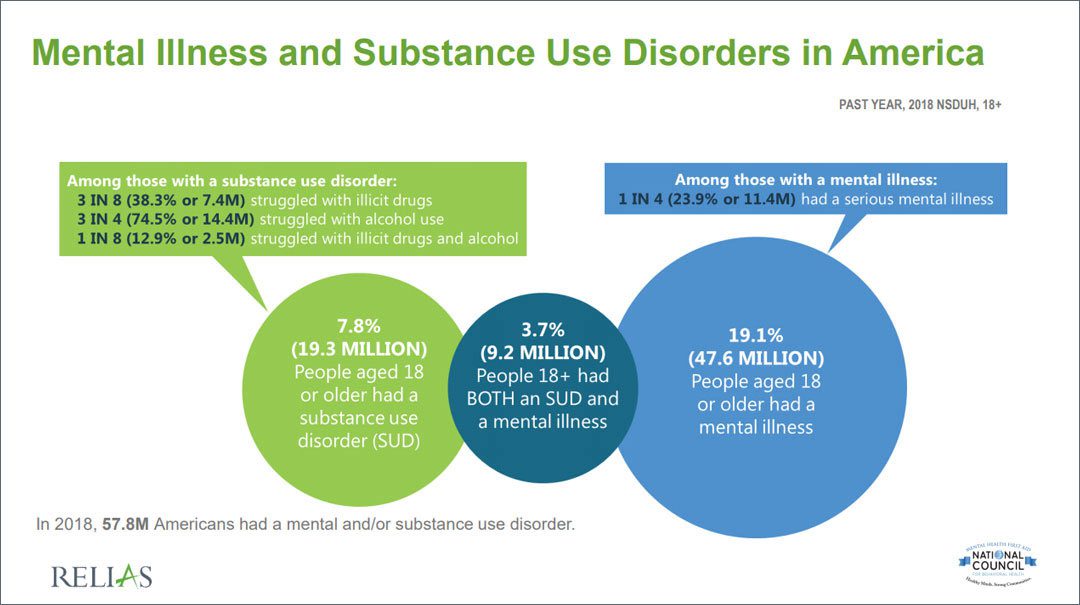
The latest data from SAMHSA and NSDUH indicate that in 2018, 57.8 million Americans aged 18 and older had a mental and/or substance use disorder.
Among those with a substance use disorder:
- Three in eight struggled with illicit drugs
- Three in four struggled with alcohol use
- One in eight struggled with illicit drugs and alcohol
Among those with a mental illness:
- One in four had a serious mental illness
In the webinar, Aaron shared more statistics regarding opioid misuse, heavy alcohol use, methamphetamine use, and co-occurring substance use disorder with suicide thoughts. This data shows the demand and need for behavioral health services, including substance use treatment.
The Current Landscape of Substance Use Treatment
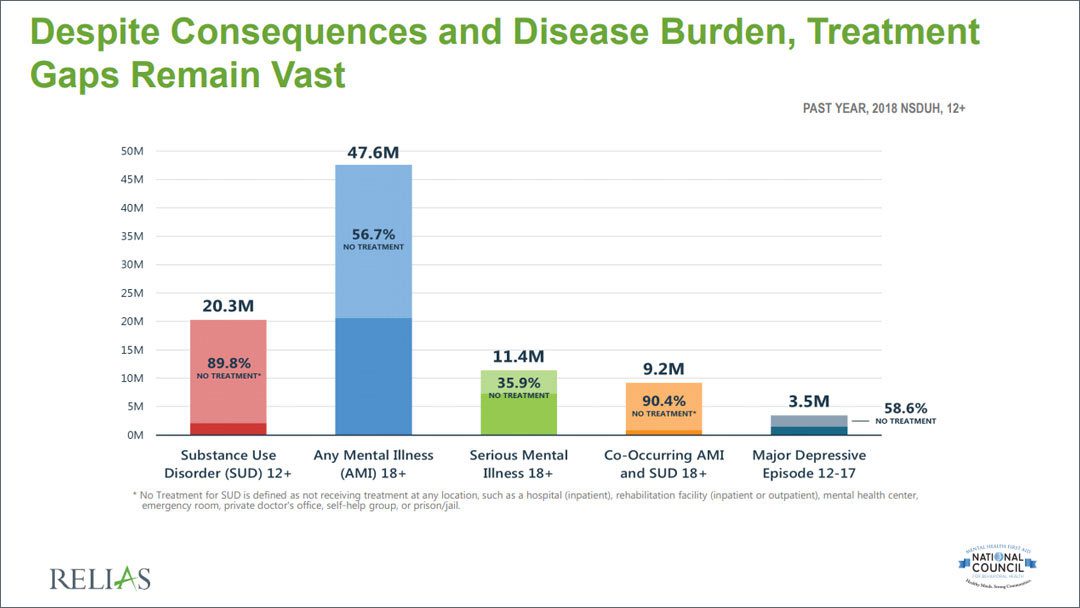
Even with all the data, there are still issues with treatment and treatment demand.
“The vast majority of people with a substance use disorder, actually receive no treatment,” Aaron says. The same is true for those with a mental illness, serious mental illness, and a co-occurrence of mental illness and substance use disorder.
Some of this can be attributed to the challenges behavioral health and substance use treatment facilities face, like workforce shortages and the ability to provide accessible treatment to clients in rural communities.
And with workforce shortages only projected to get worse — HRSA suggests that demand for addiction counselors may increase anywhere between 21% and 38% while the supply of addiction counselors will increase 6%, resulting in a deficit — it’s imperative that facilities use modern treatment models to improve quality of care and long-term sobriety outcomes.
Critical Areas of Knowledge Development
To support quality of care and long-term sobriety, Aaron highlights how the field is changing (moving from addiction as a moral failing to a chronic brain disorder), what the substance use disorder treatment continuum of care looks like, and how medication-assisted treatment (MAT) and peer support specialists are improving clinical outcomes.
Aaron also reviews areas where counselors should continue to hone their skills, for things like motivational interviewing, cultural competency, and suicide screening and assessments.

If you missed the webinar, you can watch a replay here.
Questions We Didn’t Have Time to Answer
We received many great questions during the webinar, so many that we couldn’t answer them all live. Aaron graciously answered all the questions offline and we’re sharing them below:
How do we identify gaps in our staff’s competency, so we can improve the quality of care we deliver?
I would encourage you to think holistically about this issue and look at organizational capacity as well as individual staff competencies. One of the first things I would do is assess whether my organization is offering the evidence-based interventions that provide clients with the greatest likelihood of success and long-term recovery. If not, then I would begin to implement those practices. I would also look at my supervision protocols to make sure that the appropriate supervision processes are in place to support staff.
How do we support our peer providers/specialists in their own recovery while having them provide support to clients?
In most cases, the support and care that peer specialists need is similar to what any service provider may need working in the behavioral health field. So, you want to make sure that you have programs and activities that support health and wellness and make sure that all staff have access to those programs.
Do you have any information on how culture affects recovery in SUD and usage as far as the way we address helping an individual become whole?
Culture certainly plays a huge role in the treatment and recovery process. Treatment providers should strive to be “culturally intelligent” in the implementation of all their services. SAMHSA has a number of resources that can be useful as you think through how to address issues related to culture.
Are there efforts being made to address pay inequity of substance use providers? It seems like this would address the workforce issue. Addressing provider burnout and improving work conditions would be important, too.
Salary is certainly a critical workforce issue that needs to be addressed. There are some policy initiatives that are trying to address related issues, such as student loan repayment. I agree more needs to be done in this area.
There seems to be a mixed message about recovery and 12-step programs—most treatment appears to be TSF. This seems to be in direct opposition of MAT and promotes ‘powerlessness.’ How do we in the field move away from this mindset?
My view is that, as a field, we need to focus on the use of evidence-based practices and more person-centered approaches to care. These practices will ultimately give providers and clients the best chance at a successful recovery. As a field, we have to keep our focus on those treatment options that we know are effective and double our efforts to disseminate those practices to the field.
Help Your Counselors Provide Better SUD Treatment in 2020 and Beyond
Whether you’re in charge of training, hiring, or ensuring compliance at your facility, there are things you can do to help your counselors provide better SUD treatment. Check out the resources below:

The Substance Use Professional of the 2020s
How does organizational leadership ensure that their clinical staff possess and can apply the core competencies needed for effective practice in the decade to come?
Watch the webinar →





