Despite the number of individuals affected by mental illness and mental health disorders, the stigma around mental health remains. In 2018, one in five adults experienced mental illness, while suicides have risen 31% since 2001 and are now the leading cause of death among people aged 10-34 in the U.S.
To suggest that healthcare workers are exempt from experiencing mental illness and mental health disorders would be nothing short of illogical, yet the mental health stigma is only magnified in the healthcare industry. In fact, healthcare workers face a unique level of stigma amidst the intense professional pressure to excel in the workplace.
Mental health data have even shown physicians to have a higher suicide rate than many professions (including those in the military), and are more likely than the general population to die by suicide — 28 to 40 per 100,000. In other words, one doctor commits suicide nearly every day in the U.S. alone. The complicated reality is that the stressors placed on healthcare workers are also the very barriers that can deter them from seeking treatment, creating a Catch-22 for those seeking help:
- Fear of judgement. Most U.S. state medical licensing boards include questions about mental health history. There is evidence that such questions make physicians afraid that seeking help for a mental health issue will affect their ability to practice medicine or damage their professional reputation.
- Unrealistically high standards. Certain clinical roles can hold themselves to incredibly high standards, often because of their training and competitive nature, and are less likely to admit when they need help or treatment.
- Calling to serve others. Healthcare workers commonly enter the healthcare industry with a calling to care for others and might feel unqualified to effectively care for others if they need treatment for themselves.
The Pandemic’s Effect on Healthcare Workers
The COVID-19 pandemic has unleased unforeseen stressors on healthcare workers that continue to evolve day by day. The implications of COVID-19’s impact on mental health have begun to appear in current research — studies of Chinese healthcare workers who initially responded to the pandemic have seen an increase in anxiety (almost half), depression, fear of workplace violence, and a third have insomnia.
A CDC study of 5,000+ survey respondents between June 24, 2020 and June 30, 2020 found that almost 31% of self-reported unpaid caregivers and 22% of essential workers had considered suicide in previous 30 days. Another 13.3% reported using alcohol and prescription or illicit drugs to manage stress related to the pandemic.
To make matters worse on a national level, a new study suggests that the U.S. is also experiencing more mental health consequences than people in other countries. This data suggests that American healthcare workers are experiencing greater impacts on mental health, yet to be understood and managed.
The American Psychiatric Association has discussed the likelihood of post-traumatic stress following the pandemic, recognizing the stigma around mental health preventing healthcare workers from seeking care. Healthcare workers, especially those who are directly caring for COVID-19 patients, are at a high risk of developing traumatic stress disorders due to unprecedented levels of burnout, moral injury, and compassion fatigue.
The Joint Commission Addresses Stigma
In response to the novel coronavirus pandemic, The Joint Commission issued guidance on promoting psychological well-being of healthcare staff during crisis for healthcare organizations. Noting the importance of healthcare workers’ well-being as a foundation for providing adequate patient care during a crisis, the guidance called out the fact that, “The anxiety, stress, fear and associated feelings experienced by healthcare workers during challenging times are real, justifiable, and do not indicate weakness or incompetence.”
Additionally, The Joint Commission issued a statement affirming its support for the removal of any barriers that inhibit clinicians and healthcare staff from accessing mental health care services, including eliminating policies that reinforce stigma and fear about the professional consequences of seeking mental health treatment. In fact, The Joint Commission supports the recommendations of the Federation of State Medical Boards and the American Medical Association to limit inquiries to conditions that currently impair the clinicians’ ability to perform their job and does not require organizations to ask about a clinician’s history of mental health conditions or treatment.
The timely guidance from The Joint Commission also included helpful self-care methods for individual healthcare workers, as well as strategies managers and leaders can use to support their teams, such as:
- Communicate regularly.
- Model behaviors that promote self-monitoring.
- Encourage sharing of concerns.
- Demonstrate value of staff.
- Orient staff to psychosocial resources.
- Proactively monitor and provide active outreach.
- Encourage peer support.
- Share positive feedback.
- Adapt staffing where possible.
- Resilience in post-crisis recovery.
Why Change Can’t Wait
At a time when caregivers are putting their lives on their lines more literally than ever before, society cannot continue to unfairly praise them as “heroes” without acknowledging that they are first and foremost “human beings” just like us.
Despite the research and data showing that healthcare workers are not only at an increased risk of experiencing mental health symptoms, we also know they’re less likely to seek treatment — largely because of the mental health stigma in healthcare.
Healthcare leaders are recognizing that this needs to change — and fast — as medical experts are expecting a second wave of mental health issues to hit healthcare workers after the coronavirus abates. Some are warning that a “parallel pandemic” of post-traumatic stress will beset healthcare workers who witnessed COVID-19 deaths and suffering in patients and colleagues.
While the novel coronavirus will forever change the healthcare landscape in ways leaders cannot fully predict and plan for, providing support for healthcare workers will always remain a leading priority. Organizations and individuals alike can (and should) make a conscious effort to help change the perception of mental illness and mental health disorders as a critical first step to reducing the stigma.
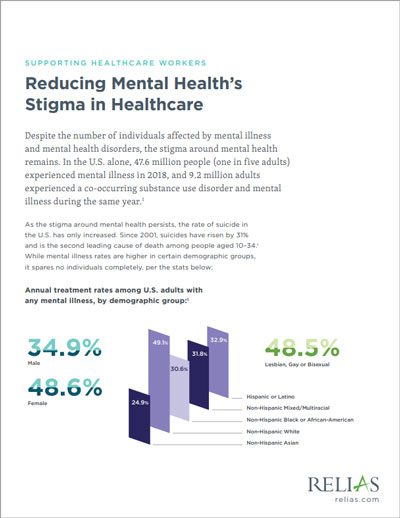
Reducing Mental Health’s Stigma in Healthcare
Despite the number of individuals affected by mental illness and mental health disorders, the stigma around mental health remains. Download this white paper to learn how to reduce the stigma, through education, transparency, compassion, and advocacy.
DOWNLOAD THE WHITE PAPER →





