Despite the leaps and bounds made in healthcare in recent decades, the maternal mortality rate in the United States is still jarringly high. What, exactly, is the U.S. rate? As of 2018, the U.S. maternal mortality rate was 17.4 per 100,000 live births, amounting to 658 lives lost as a result of complications associated with pregnancy in 2018. According to the World Bank, the U.S. rate is higher than the maternal mortality rates of 56 other countries. In fact, the U.S. is the only developed country in which the maternal mortality rate is steadily increasing.
As the maternal mortality rate in the U.S. continues to rise, hospitals across the country must establish evidence-based plans designed to reverse the course of this national crisis.
What Is Maternal Mortality?
The World Health Organization (WHO) defines maternal mortality rate as the number of mothers who pass away during pregnancy or within the six weeks after a pregnancy is complete. The “completion” of a pregnancy can indicate either a delivery or an abortion. Maternal mortality does not include accidental or incidental deaths — a mother’s death must be related to her pregnancy or a complication of obstetric care to be considered a maternal mortality.
High maternal mortality rates are unevenly distributed across the globe, with the highest concentrations occurring in low- and middle-income countries. According to the WHO, 86% of the roughly 295,000 global maternal deaths in 2017 occurred in Sub-Saharan Africa and South Asia. By contrast, many developed countries like Iceland, Italy, and Poland typically report extremely low maternal mortality rates (between 2% and 4%), indicating that maternal mortality can be prevented with a robust and well-funded maternal healthcare strategy.
But despite the prevalence of maternal mortalities in Sub-Saharan Africa and South Asia, both regions experienced a significant drop in their maternal mortality rates—40% and 60%, respectively—between 2000 and 2017. While these metrics imply a promising future for maternal health outcomes in developing countries, they also reveal just how unusually severe the United States’ maternal healthcare crisis is.
What Are the Causes of Maternal Mortality?
With a firm grasp on what maternal mortality means, we can dig deeper into the causes of maternal mortality. Maternal mortality is most commonly associated with complications during delivery, but it can also occur as a result of unsafe abortions or chronic conditions that affect a woman’s postnatal health like diabetes.
It’s important to note that the causes of maternal mortality often vary from country to country. In hospitals with limited access to sterilized equipment, postnatal infections like sepsis are more common. While sepsis can still occur in the U.S., it is not the leading cause of maternal mortality.
What is the leading cause of maternal mortality in the U.S.? Cardiovascular conditions. Cardiovascular conditions like heart attack and stroke as well as obstetric hemorrhages, eclampsia, obstructed labor, and ill-advised caesarean sections can put a woman’s life in jeopardy.
Cardiovascular Conditions
Cardiovascular conditions account for more than 33% of all pregnancy-related deaths. While some of these deaths are associated with preexisting cardiovascular conditions, the majority are a result of heart conditions that developed during pregnancy. Pregnant women experiencing shortness of breath, chest pain, palpitations, or fluid retention must be tested for heart disease in an effort to minimize complications.
Obstetric Hemorrhage
Obstetric hemorrhages (excessive bleeding) account for approximately 25% of maternal deaths worldwide, making hemorrhaging one of the leading causes of maternal mortality. More than 80% of obstetric hemorrhages occur postpartum, but it’s important to note that excessive bleeding can occur at any point during pregnancy. While the most severe cases result in death, the majority of women fully recover from obstetric hemorrhages.
Eclampsia
Eclampsia is the onset of seizures as a result of high blood pressure. Eclampsia can occur at any point during pregnancy, but it is most prevalent during childbirth. Eclampsia rates are especially high in the U.S., where a large percentage of women experience hypertension and obesity — two significant risk factors for the condition.
Maternal mortality from eclampsia can be minimized through close monitoring of patients with preexisting hypertension as well as early detection of hypertension developed during pregnancy.
Obstructed Labor
Often associated with infant mortality, obstructed labor can also lead to maternal mortality. Obstructed labor occurs when a blockage prevents the infant from properly exiting the womb. While many obstetrics teams are well-trained in managing obstructed labor to ensure infant survival, complications for the mother—including eclampsia and hemorrhages—often go undetected.
Obstetrics staff need access to in-depth training and education on the potentially fatal effects of obstructed labor for women to help ensure the health of both mothers and children during these life-threatening situations.
Overuse of Caesarean Sections
Caesarean sections (C-sections) became commonplace during the 1960s with the introduction of improved antiseptics and surgical technology. By 1990, nearly 23% of births in the U.S. were performed using the procedure.
As C-section rates grew during the late 20th century, so did awareness of the risks associated with the procedure. Compared to vaginal birth, C-sections result in higher instances of maternal mortality, longer hospital stays, and excessive bleeding. Yet despite these risks, C-sections have continued to increase in popularity among patients—even when the procedure isn’t medically necessary.
Due to the heightened risk of maternal mortality, medical professionals and expecting mothers alike need access to comprehensive information about the procedure. Every member of the obstetrics care team should be well-informed of the risks associated with C-sections and empowered to communicate those risks to their patients.
Why Is U.S. Maternal Mortality So High?
To improve maternal health outcomes, obstetrics care professionals need to understand the answer to one fundamental question: Why is maternal mortality so high in the U.S.? The high rate of maternal mortality in the U.S. is the result of a complex combination of factors, including those related to variations in care, a social preference for C-sections, and socioeconomics.
Variations in Care
Variation in care across hospitals accounts for a wide range of preventable maternal health complications. Some healthcare institutions don’t have access to a large pool of highly skilled obstetrics employees, some lack effective communication strategies and leadership, and some don’t have the funding to purchase advanced technology and equipment. In many cases, an institution may face all of these challenges and more.
But, more often than not, variations in care in the obstetric ward are rooted in a profound misunderstanding surrounding the value of emergency maternal care training. When clinicians are ill-prepared to prevent, detect, and respond to maternal emergencies, maternal mortality is more likely to occur.
Follow-up protocols create another avenue for significant variation in maternal healthcare. As noted above, maternal mortality isn’t just a measure of mortality during childbirth—complications up to six weeks after birth contribute to high mortality rates around the world. Common postnatal complications include postpartum hemorrhaging, sepsis, and exacerbated hypertensive disorders. To limit the risk of these complications, hospitals must conduct regular, comprehensive follow-ups with a mother in the weeks immediately following the completion of her pregnancy.
Social Preference for C-Sections
A variety of factors lead to the high rate of C-sections in the U.S. For many working women without access to robust maternity leave benefits, the precise scheduling of the procedure is not only a convenience, but a necessity. Additionally, many American women believe C-sections are less risky and more technologically advanced than vaginal birth.
The WHO and the Centers for Disease Control and Prevention encourage physicians to promote vaginal birth unless a C-section is deemed medically necessary. When hospitals deploy an effective, uniform strategy to combat overprescribed C-sections, they can help significantly reduce the risk of maternal health complications among their patients.
Socioeconomic Factors
Around the world, low-income areas have the highest prevalence of maternal mortality, and the U.S. is no exception. In fact, much of the interstate variance in maternal mortality rates across the U.S. can be attributed to complex socioeconomic factors.
While socioeconomic factors can be difficult for many healthcare professionals to address, it’s important for these professionals to understand the large-scale factors that contribute to maternal mortality among certain populations.
Extensive travel to medical facilities and preexisting health conditions, including hypertension and obesity, disproportionately affect women in low-income areas. Additionally, patients working in low-wage jobs that offer little to no paid maternity leave may be more likely to request a medically unnecessary C-section to ensure they can remain employed for as long as possible. Mothers with low incomes are also less likely to request follow-up visits, as these visits aren’t always covered by healthcare providers or insurers.
Race is another socioeconomic factor contributing to increased maternal mortality in the U.S. According to a study published in the National Library of Medicine, black women are three to four times more likely to experience a pregnancy-related death than white women are. Societal and health system factors including higher rates of hypertension, income inequality, and lack of access to high-quality care all contribute to this devastating reality. Combined, these factors help explain why states with large populations of black Americans register some of the highest rates of maternal mortality in the country.
How to Reduce Maternal Mortality and Save Mothers’ Lives
The complications associated with pregnancy are often preventable with the right tools, precautions, and training. During every phase of delivery, all members of the maternal care team—nurses, doctors, midwives, and so forth—must vigilantly watch for signs that the mother is in danger. When a hospital does everything in its power to minimize maternal fatalities, providing women with a safe, supportive environment, it establishes its reputation as a competent, trustworthy healthcare provider.
But which intervention is most critical for preventing maternal mortality? Every case is unique, and yet uniform, evidence-based reforms to obstetric care can help drastically reduce fatal complications associated with pregnancy. The three steps outlined below are designed to help obstetrics professionals minimize variations in obstetric care and provide all mothers with the informed, knowledgeable care they deserve.
1. Be Prepared
To quickly address a maternal emergency, clinicians must be prepared for the worst-case scenario at all times. Preparation involves uniform education that addresses risk factors for fatal conditions as well as emergency response procedures. With this information in hand, everyone on the obstetrics care team is prepared to spot the warning signs of issues early and jump into action as soon as symptoms start to manifest.
To detect and prevent obstetric hemorrhages, healthcare professionals must measure 100% of the blood lost during C-sections and vaginal births. Delivery units must be stocked with a blood bank that can support a massive transfusion if required and have all pertinent medications readily available. Obstetrics departments are also encouraged to designate a hemorrhage response team equipped with the skills to address a hemorrhage on a moment’s notice.
For rapid response to eclampsia and other hypertension-related conditions, obstetrics care teams must be equipped with intravenous hypertension medication and magnesium sulfate to mitigate seizures. Access to modern healthcare equipment—including telemedicine technology for rural areas—is also vital. With the right tools, healthcare professionals can regularly conduct pre- and postnatal follow-ups and identify risk factors early.
2. Know the Warning Signs
All members of the maternal care team must monitor for obstetric hemorrhages as soon as labor begins to ensure blood loss is kept to a minimum. That means ensuring hospital staff know how to identify preexisting risk factors for obstetric hemorrhages as well as the signs that a hemorrhage has occurred, including low blood pressure, dizziness, and nausea.
It’s also important for clinicians to regularly monitor the mother’s blood pressure throughout her pregnancy and especially during delivery. Those with preexisting risk factors for eclampsia must be monitored particularly closely. When healthcare professionals know how to prevent maternal mortality through early detection, the rate of mortality is drastically reduced.
3. Promote Vaginal Birth
Due to the higher risk of maternal health complications associated with C-sections, maternal healthcare experts within the U.S. and across the globe are encouraged to advocate for a vaginal birth when a C-section is not medically required.
Education is paramount when it comes to increasing vaginal births. Healthcare institutions across the U.S. must adopt a robust educational program that ensures all their obstetrics professionals have a sound understanding of C-section target rates as well as the research supporting vaginal birth. Education is also important for expecting mothers, who often believe C-sections are more advanced, safer, or easier than vaginal births. To reduce variation in C-section rates among hospitals, a comprehensive educational and promotional approach is key.
How Relias Can Help
Every hospital has a part to play in reducing the rate of maternal mortality. To minimize variation in care, hospitals must embrace evidence-based obstetrics education that facilitates a uniform approach to treatment. This type of approach eliminates ambiguity and provides healthcare professionals with the skills to quickly identify and treat the causes of maternal mortality.
Relias Obstetrics (Relias OB) is an assessment-driven education and analytics solution designed to help healthcare providers identify and reduce variation in care where it matters most. Relias OB casts a wide net, helping improve clinical practices and clinical outcomes in every part of the delivery room by providing all members of the obstetrics care team with critical maternal mortality insights.
How to Utilize Relias OB
Relias OB’s research-based educational framework allows obstetrics care teams to approach maternal care with a unified strategy outfitted with the most effective maternal mortality prevention tactics. Hospitals that use Relias OB have seen reduced variation in obstetric healthcare, improved maternal health results, and advanced skill development among their staff. In fact, our clients report improvements in massive blood transfusion protocols of 50% as well as 46% reductions in eclampsia cases—a clear indication that Relias OB successfully improves patient outcomes.
Relias OB’s personalized learning strategy homes in on five of the most important maternal health action areas: assessing and monitoring the fetus, recognizing and treating obstetric hemorrhages, addressing hypertensive disorders, promoting vaginal birth, and treating shoulder dystocia. For each of these areas, Relias OB provides a comprehensive educational program that prepares physicians and nurses with the skills they need to prevent, detect, and address emergencies in maternal healthcare.
Reducing maternal mortality and improving maternal health requires every hospital to take an evidence-based approach to maternal care. The courses offered by Relias OB have been validated by the Association of Women’s Health Obstetric and Neonatal Nurses and accredited by the American Nurses Credentialing Center and the Accreditation Council for Continuing Medical Education. To learn more about how your hospital can use Relias OB to improve maternal health outcomes, visit our website.
Editor’s note: This post was originally published in June 2020 and has been updated with new content.
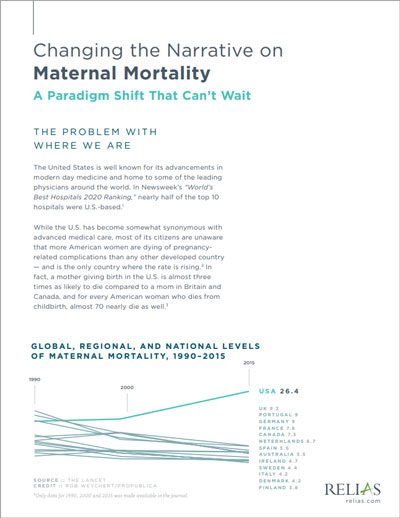
Changing the Narrative on Maternal Mortality: A Paradigm Shift That Can't Wait
The U.S. is faced with an urgent call to improve maternal care. This white paper outlines where we are as a nation, where we need to go in terms of improvement, and how to get there.
Download White Paper →





