In the past decade, employment in the field of long-term care has seen substantial growth. And that’s not expected to change any time soon! Employment opportunities in healthcare in general are expected to grow 19% between 2014 and 2024, per the U.S. Bureau of Labor Statistics. (For reference, average job growth across all job sectors is just seven percent.) Jobs such as home health care aids, physical/occupational therapy aids/assistants, are expected to grow even more, with projected growth of 38% and 40% respectively during the same period. Wow, talk about job security.
Unfortunately, we also have another “gift” that comes along with high-growth: high turnover rates.
Despite the rosy picture of increasing demand, healthcare also has a supply problem with workers leaving healthcare settings at rates that outpace other industries significantly. Turnover rates for nurses and aides can range from 55% to 75% and are even worse for aides alone. When people leave the field faster than enter it, the situation becomes difficult to address.
The following graphic, from a 2015 Long-Term Care Research Report from the UCSF Health Workforce Research Center illustrates this disparity quite clearly. The delta between the blue and red bars spells catastrophe for the long-term care industry if left unaddressed. It’s just not sustainable.
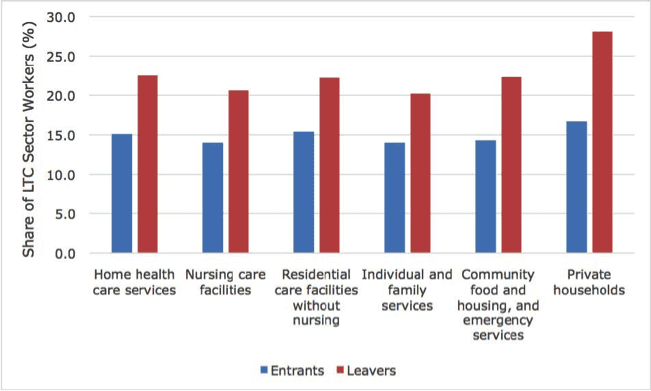
Here’s another thing, long-term care leavers tend to report higher rates of work disability and to have higher rates of poverty.
The impact of this turnover on an organization’s bottom line is significant and measurable. In fact, it can be upwards of 30% of an employee’s annual salary. In real terms, if a caregiver’s compensation is set at $23,000 per year, the cost of replacing that position is almost $7,000, multiplied by the number of positions needing to be replaced each year!
On the flip side, this also represents an opportunity for improving your bottom line by reducing turnover. One study of 902 nursing homes in California found that even a ten percent reduction of turnover could save nearly three percent of total costs (upwards of $165,000 per facility).
Training new staff is hard and providing the continuous training and support to keep staff happy is hard. But it’s also necessary and needs to happen both at the C-level and the community level. Most executives understand this dynamic, but managers at the community level are faced with balancing limited time, available resources, and the day-to-day demands of running their organizations.
Those leaders in the executive offices need to step up and do the following:
- Begin with a thorough analysis of the problem. You can’t manage what you don’t measure, so here are two resources to get started:
- Get familiar with the topic of job embeddedness. What is it? It’s all about the fit of new hires between themselves, the organization and the specific jobs they are hired for.
- Get ready to invest in ongoing staff education and training. Well-crafted training programs not only improve the job skills of direct-care workers but also reduce occupational injury rates and job turnover.
- (Re)consider your budgeted training hours. It’s surprising the mismatch between what new hires need and what budget hours allow. It might be time for some realignment of your budget.
- Think seriously about your current management training and their role in supporting and training new hires. Stacks of DVDs out of context does not make for a welcoming orientation. We can do better!
- Don’t go it alone. Consider the expertise of training professionals when you design your training programs and approaches. They are experts in translating what workers need to know into terms they can understand and embrace.
- Increase the number of workers per resident. This is a tough one. Consider this finding from a 2007 Donoghue and Castle study: Increasing the number of aides per resident from 33 per 100 to 41 per 100 reduced CNA turnover from 65% to 41% and also lowered LPN and RN turnover. And with proposed competency-based regulations, staffing (and training that level of staffing) will come more closely into focus.
Henry Ford said it best: “If you always do what you’ve always done, you’ll always get what you’ve always got.”
The stakes are too high. We must address this issue head-on (and quickly)!






