Online education and competency management tools that ensure compliance and elevate care quality
Post-acute care organizations improving outcomes with Relias
Learn how Relias helps our clients every day.
Relias helped four CalVet nursing homes earn five stars on Medicare.gov’s Care Compare website.
“I have seen the direct correlation of enhanced training curricula and how it helps in passing our surveys and inspections and achieving the highest ratings possible.”
Miguel Mojado, MSN-INF, RN, DSD
Supervising Registered Nurse/Nurse Instructor at Veterans Homes of California (CalVet)
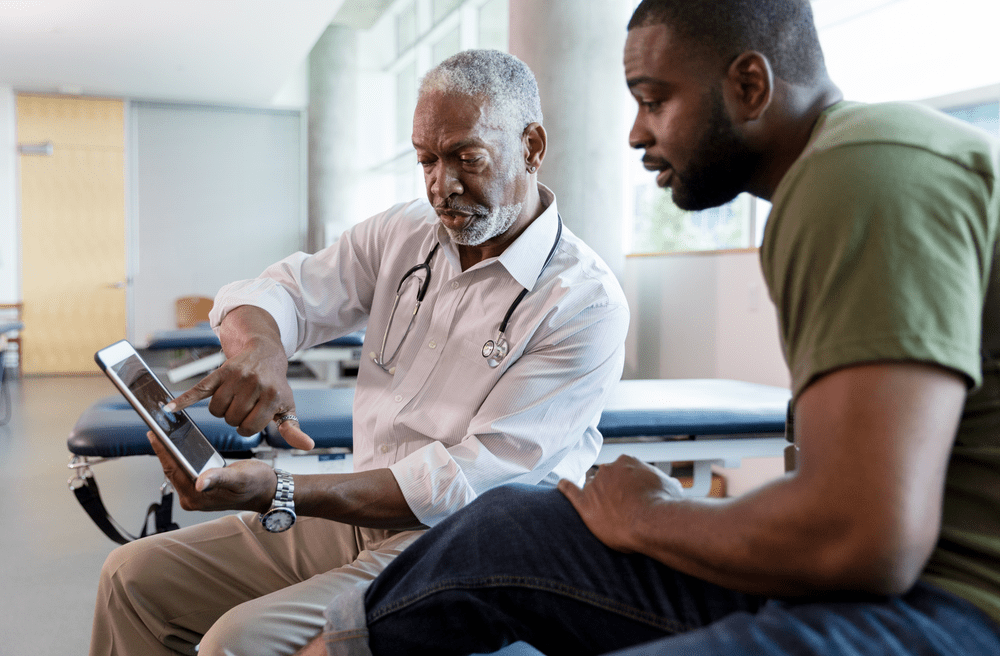
Relias is Common Sail’s partner in growth.
Common Sail Investment Group’s portfolio includes independent living, assisted living and memory care, home health, hospice, home care, pharmacy, healthcare staffing, and even construction. Hear how Relias has been Common Sail’s partner in growth as they’ve expanded from 14 senior communities in one state to 115 communities across nine states.
Find out other ways Relias helps CSIG navigate change and growth by reading their full success story.
Not sure where to start?
Connect with us to understand how our solutions can help your organization.



















